Rotator Cuff Repair Surgery
Rotator Cuff Repair Surgery
Information Regarding Rotator Cuff Repair Surgery
1. The Problem
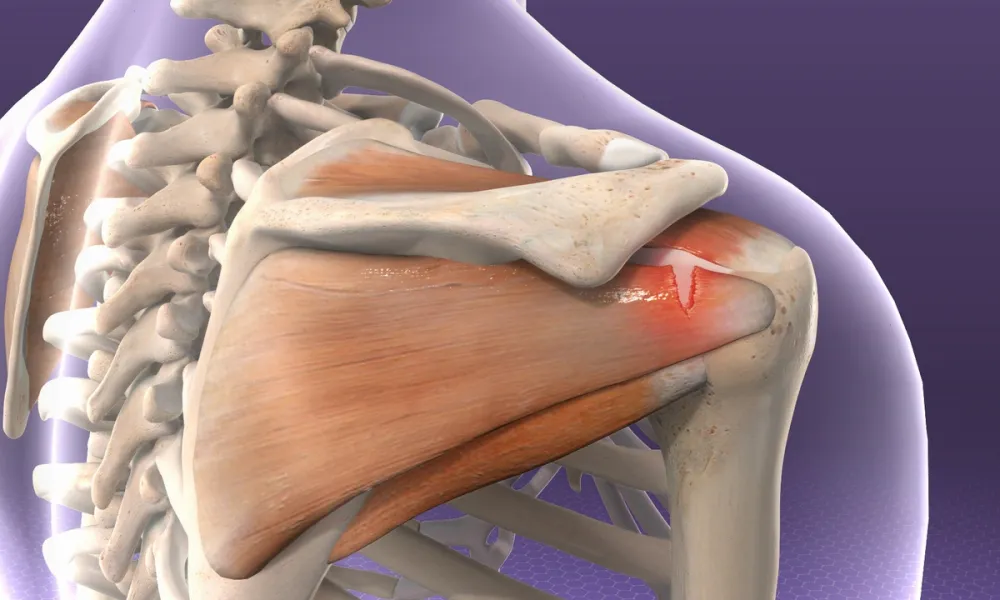
The rotator cuff is a group of four tendons that help to move and
stabilize the shoulder. Rotator cuff tears are a common cause of
shoulder pain and disability. Rotator cuff tendons tears can occur as
the result of injury (falls or heavy lifting) or as the result of "wear
and tear" and aging changes that significantly weaken the tendons thus
placing them at increased risk for injury.
Individuals with rotator cuff tears usually experience shoulder pain and
weakness. Rotator cuff tears usually get worse over time leading to
greater pain and disability.
2. The Repair
The goal of the rotator cuff repair surgery is to securely attach the
tendon to the bone from which it was torn. We believe this goal is most
reliably accomplished through a limited "mini" surgical incision usually
2 to 3 inches in length. The repair is performed with sutures (lengths
of surgical thread) that pull down and hold the tendon edge on to the
bony surface to which it then will heal.
An important goal of surgery is to ensure smooth passage of the
repaired cuff beneath the overlying bony shelf known as the acromion.
This often requires the removal of bony prominences from under surface
of the acromion thereby providing greater room for smooth clearance of
the repaired cuff.
Occasionally the detached rotator cuff can be repaired with arthroscopic
anchor techniques. However, it is not clear that this technique offers
advantages over or is as reliable as a direct open repair performed
through a limited incision. Some studies have demonstrated a higher
failure rate after arthroscopic rotator cuff repair surgery.
3. Effectiveness
Rotator cuff surgery usually results in significantly improved shoulder
function and comfort that is reliable and long lasting. The
effectiveness of the procedure depends on many factors including the
health and motivation of the patient as well as the condition of the
shoulder at the time of surgery. It is important to recognize that
surgery cannot improve the basic quality of tendon tissue. Chronic or
massive rotator cuff tears are often severely scared and retracted.
These tears may be irreparable. Even when the tendon defect cannot be
fully repaired, removal of scarred tendon and bony prominences can
result in significantly improved shoulder comfort.
4. Surgical Risks
The risks of rotator cuff surgery include, but are not limited to,
infection, injury to nerves and blood vessels, stiffness of the joint,
re-tear of the repaired rotator cuff, and persistent pain.
5. Preparation For Surgery
Patients should optimize their health to improve their chances of a
successful outcome. Smoking should be stopped a month before surgery and
not resumed for at least 3 months afterwards. Smoking interferes with
the healing of the rotator cuff and the ultimate strength of the repair.
Before surgery, you may require medical clearance from your regular doctor if you have medical problems. You may be required to obtain some basic tests for screening before the surgery. Basic blood tests, a chest x-ray, and an EKG may be required depending on your health.
6. Protecting Your Repair
The patient's motivation, cooperation and activity modification are
critical elements impacting the success of rotator cuff repair surgery.
We recommend strict sling protection for 12 weeks post repair. Numerous
studies have documented that it takes 12 weeks for the repaired tendon
to heal to bone. Premature use of the arm will place the repair in
jeopardy.
One of the major goals of rotator cuff repair surgery is to maintain flexibility in the immediate postoperative period. To accomplish this, your surgeon will prescribe protected range of motion exercises beginning within a day of two after your surgery. In general, these exercises can be performed at home. We recommend these exercises be performed every 3 to 4 hours (4 to 5 times a day).
It is important that the repaired tendons not be challenged until they have had a chance to heal. We recommend that you make no attempt to engage the repaired arm away from the side of the body, i.e. absolutely no reaching or lifting activities for a full 3 months. Light finger activities such as keyboarding, shuffling cards, buttoning your shirt will be permitted and may be initiated within a few days after surgery.
At 12 weeks after surgery you will be permitted to wean the use of your sling and resume light use of the repaired shoulder. With the consent of your surgeon, patients may be able to return to activities such as swimming, golf and tennis -usually approximately 4 to 5 months after the surgery. Recovery of comfort and function after rotator cuff surgery continues for up to a full year after surgery.
7. Returning to Work
Your return to work depends on your profession and the availability of
"light duty" work. Generally, light office work, i.e., typing, writing,
and the use of a computer may be started as early as 2 to 3 weeks after
surgery.
8. Long term limitations
Patients should avoid activities that involve extreme heavy lifting, and
other major impact such as contact sports or activities that
significantly increase the risk of falls. These activities may increase
the chance of repeated injury to your rotator cuff repair.
9. Problems?
Call your surgeon if you have an elevated temperature greater than 101.5
degrees, redness or drainage from the incision site as these changes
may be early signs of a wound infection.
If you are running low on pain medication after surgery and anticipate the need for more, please call your doctor's office during regular office hours (8am to 5pm Monday -Friday) well in advance of running out of pain medication. Pain medication needs must be handled through our office. Pain medications needs cannot be addressed after hours or on weekends.
10. Summary
Rotator cuff surgery is a very effective and reliable method for
restoring comfort and function to shoulders with rotator cuff tears.





